I’m so grateful to BabyCenter for taking on this huge and extremely sensitive subject of cesarean. If you’re interested in supporting me somehow, please comment at the bottom of the article and/or share it from one of their social media links at the top of the article. Muchas Gracias! This has been a long time coming for me, so I’m thrilled to have it out in the world today! Happy Cesarean Awareness Month!
Viewing entries in
Home Birth
"This is MY baby. This is MY baby," I repeated over and over in my head right before each wave to push consumed me. The urges were so strong that I felt like I could loose my breath completely.
The sun shown bright and I listened to the neighborhood children play outside as I labored calmly in my birth tub. I had wonderful rests between surges where I listened to birds and dosed off to sleep. My doula whispered, "You are having a beautiful birth, Thais."
I was, but I also struggled with doubt the whole time. I was scared that I might not be able to pull it off. Even when West's head had crowned, I thought that he would get stuck and
would have to transport me to the hospital for another cesarean. And then, the hospital would have birthed by baby not me. But somehow, I managed to overcome those doubts right before each surge with my simple chant, "This is MY baby." Sometimes I would say, "Let's just get through this next one. Just one more."
The realization that only I can birth my baby in the way that I want was an on going theme for me throughout my pregnancy. People that I felt dependent on and wanted at my birth didn't work out for one reason or another. Even Maria had to go lobby in Washington on my due date, and I had to come to terms with the fact that she might not be there for the birth. Luckily, West came when she got back. I am so grateful for that.
For my first son's birth, subconsciously, I always thought that I'd be saved like Cinderella is saved from her evil step-sisters. I assume that it is a cultural message ingrained in my psyche since I was a little girl. It's important to have support, but the reality is that only the Mama can birth the baby. It is hard to be alone on such a hard journey, but the belief that I could do it and my two years of preparation allowed the baby to come. I pushed as hard as I possibly could. I wanted him to arrive protected at home and in peace.
"This is MY baby," I chanted over and over again to myself. And I did push him out. He came right out like he should. It took only one hour of pushing after seven hours of active labor. Baby West was born at home on a gorgeous, sunny day. His demeanor is as peaceful and calm as the way that he joined us. And, he is so loved by me and so many others who have followed my recovery from my first son's birth to the discovery and actualization of a home birth with my second. When Maria put him on my chest, I rejoiced, "I did it! I did it!"
, my doula, cried with joy next to me as she listened to my reaction. I feel so powerful. Birth really is empowering.
As I celebrated holding my new baby in my arms and watching him nurse perfectly without any instruction. Maria said, "Now that is an unmedicated baby." After a brief celebration, Maria was looking serious again because I still had not birthed my placenta. We waited an hour and tried everything from angelica root, to nursing, to a shot of pitocin. Finally Maria had to make the decision to call 911 and have an ambulance transport me to UCSF. I needed a manual removal of the placenta. It was only Maria's fifth ambulance transport in her 23.5 years of being a midwife. Four of the five transports were placenta related.
Maria can perform the procedure herself, but since I had had a previous cesarean the chance of hemorrhaging was too risky. The procedure at UCSF was short and I was back at home shortly afterward. I am happy to have had a good hospital experience rather than one of a victim. It was a necessary part of my healing.
As Maria and I waited for Zack to pull the car around in the quiet lobby of the hospital at midnight, she said, "This is what home birth is all about, it's a collaboration with the hospitals. We come to them when we need their services and we only use what we need."
Please join the MAMA Campaign to help lobby to include Certified Professional Midwives in the Obama's Health Care Reform bill.
All went well and I had my beautiful baby at home on my side of the bed. I used the tub but it wasn't where I chose to birth my baby for whatever reason. I was in active labor for seven hours and pushed for one hour. He latched on right away and I had a glorious hour with him before I had to go to the hospital for a manual removal of my placenta. The procedure was short and I was back home in bed with my baby shortly afterward. I feel like the hospital experience was a vital part of my healing, but I am glad that it was a short and relatively easy visit.
I am writing a more detailed birth story for this blog and
's blog. It will still be abbreviated. I really need to write a book to cover the full two years of my experience.
I am sure happy to be on the other side and to have had a successful and joyful birth experience. What a load off! Time to move on but not from the home birth community; I am here to stay.
West weighed 8lbs. 10 oz. He was 21 1/4 inches long. And, had a head of 13 3/4 circumference.
More about my home birth journey
.
By scheduled, I am assuming that they mean scheduled for induction of labor. I am truly surprised by the number of people who ask this question.
How did this become the socially acceptable response?
Why don't people say things like, "Oh that's wonderful, best of luck for a healthy baby."
As I write that phrase, I think to myself, "Of course, people must say that nice cliche phrase. "
Sadly, they really don't. Instead when they hear that my due date is tomorrow, their eyes pop out of their head and they look at me in dread and fear. They can't believe that I am at my son's swimming lesson or the grocery store or walking the Lyon St. steps.
Why do we react this way?
It is not beyond me that I am sheltered from our mainstream world of fear-based maternity care. If I were receiving care from an OBs office right now, I would surely be pressured to schedule an induction date or rather in my case a cesarean date (induction shouldn't be done with VBac mamas). I am so happy not to have that pressure and to be allowed the time and space to have my baby when my baby is ready to be born. I am certainly ready as most women are at 40 weeks. I hope he comes soon.
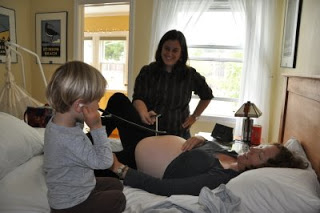
, my home-birth midwife, came over to walk through our home to get a sense of the space where my baby will be born. We have to move a couple pieces of furniture; but otherwise, we are ready. All our supplies are labeled and in the birth room (our sun room/baby's nursery). I love this picture of Mikey listening to the baby's heart beat during my check-up.
Mikey crawled in between my legs multiple times reenacting birth. He was born by cesarean so maybe it's how he knows birth to happen through images that he has seen. Or, maybe he is acting out how he would have liked to be born. Maria suggested that I watch a movie called "What Babies Want." She said it has video clips of the same behavior that Mikey was doing while I was laying on the bed. Sort of interesting.
I had false labor last night. I thought that I'd have a baby this morning but no such luck. Zack's picking up the birth tub today so we'll be having a hot tub party in our sun room tonight to give it a test run before the big event.
I'd always go alone when I first started seeing Maria Iorillo for my prenatal care. We have a three-year old and it just made sense to have my husband stay home with him. My first pregnancy, I was use to waiting an hour or more for our prenatal appointments and then only visiting for ten minutes with our care provider. I would write out my questions before my appointment because it was nearly impossible to remember them all under the stress of knowing three other mommies were waiting for their hour late appointments too.
In Maria's office, I never wait. I am greeted right when I walk in the door and sit on a couch across from a small area with wooden toys including a lovely cradle with a baby doll in it. Maria didn't need to say that children were welcome at her appointments.
Right before my third trimester, I started asking the grandparents to watch Mikey so that Zack and I could both go the appointments. As I grew more and more comfortable with my long, stress-free appointments. I invited Mikey's grandparents to come and meet Maria. So one beautiful sunny San Francisco morning Mikey, Mikey's grandparents, Zack and I all showed up for my appointment.
Maria smiled and welcomed the grandparents and Mikey to sit on the love seat next to Zack and I. She didn't ignore them and continue with her routine appointment with us, but instead said, "When grandparents come to an appointment, I like to ask them to share their birth stories." So while Mikey played with the baby doll and peered out the window watching for each Muni train to pass taking its passengers to work. Zack's mom told Maria about the birth of each of her two children at Kaiser in San Francisco in the 70s. Then, Barbara asked Maria a couple of questions about newborn care right after birth and Maria took her time to answer them. I never felt like she was rushing them out nor annoyed by their presence. After about a half an hour, the grandparents left with Mikey and Zack and I finished our appointment with Maria by checking the baby's heartbeat, my blood pressure, pulse, and weight. After that wonderful experience, we now take Mikey with us every visit so that he can be apart of his brother's birth as well.
My other posts on home birth:
On my blog:
http://www.spinachandhoney.com/search/label/Home%20Birth
On SFGate:
Read some of my other posts about birth here, here, here, here and here,and here.
Read the full article at BBC News online:
http://news.bbc.co.uk/2/hi/health/7998417.stm
Read more about this study in this opinion piece:
http://www.independent.co.uk/opinion/commentators/annalisa-barbieri-i-gave-birth-at-home-ndash-and-heres-why-1669309.html
children alone because her husband was always off working somewhere
far away and no one lived remotely close to them. The more that I digested her story the more that I realized how simple and perfect birth really is.
Birth is made to happen alone if need be. Clearly this woman was brave to be totally alone, but all women who give birth are brave. But it is reassuring that it can happen and our bodies know how to do it. It is a clean seamless process. Nothing needs to be "done" to you. The process needs to be allowed to happen freely. The umbilical cord doesn't even need to be cut at the end. It will detach itself when it dries up after a
couple of weeks like the stub does that we are all use to falling off our babies.
Processing and thinking about that pioneer woman in the woods giving birth alone to her children was one of the moments that contributed to the success of my home birth after cesarean. I remember thinking. "It's sort of crazy how long it has taken me to filter out all of what I've learned about birth so that I can finally see how simple, natural, and beautiful it is and how terribly complicated and frightening our culture has made it."
Instead of the obstetrician model of care, I am choosing the midwifery model of care; instead of a hospital birth, I am choosing a home birth; instead of taking the McMoyler Method childbirth class, I am taking Shelley Campbell's hypnobirth class; instead of no doula, I am hiring a doula.
Now that I know what I am up against, I want all the support that I can get. Having a midwife is not enough. I had a midwife for my first birth experience and she wasn't with me the whole labor like I thought that she would be. Most midwives are focused on vitals and technical things. They are very supportive and knowledgeable but work on the big picture rather than working with each surge. I understand this now and respect their role. They save their energy for catching the baby and any emergency that may come up.
A doula's only job is my comfort and to be by my side the whole time with each surge. I understand the difference between a doula and midwife now that I've experienced childbirth for myself and appreciate the importance of each of their roles during childbirth.
My childbirth experience could be fast since it's my second child. I might not need a doula, but I am thinking of it like insurance. If I need extra support to help me through transition or driving to the hospital or any other difficult situation that may arise, I want someone there to help me through it.
Mikey was pulled out of me via cesarean at the final hour, and I think that if a similar situation were to happen, a doula could help me better transition from labor to surgery to avoid some of the trauma that I suffered the first time around. Or she might be able to help me ask for more time to deliver my baby naturally. I now know that the power of birth and the hospital are so overwhelming that any bit of help is extremely valuable and could help to postpone or avoid surgery.
In their book, Mothering The Mother: How a Doula Can Help You Have a Shorter, Easier, and Healthier Birth, Marshall Klaus, John Kennell and Phyllis Klaus summarize scientific studies which have been carried out on the advantages of doula-assisted births.
Benefits from the presence of a doula:
- Reduced the overall cesarean rate by 50%
- Reduced the length of labor by 25%
- Reduced oxytocin use by 40%
- Reduced the use of pain medication by 30%
- Reduced forceps deliveries by 40%
- Reduced requests for epidural pain medication by 60%
- Reduced incidences of maternal fever
- Reduced the number of days newborns spent in NICU (neo-natal infant care unit)
- Reduced the amount of septic workups performed on newborns
- Resulted in higher rates of breastfeeding
- Resulted in more positive maternal assessments of maternal confidence
- Resulted in more positive maternal assessments of maternal and newborn health
- Resulted in decreased rates of postpartum depression
I want my only job to be birthing my baby. I don't want to worry about what is happening around me. I want my doula to filter out the drama and deliver the truth to me in raw form. I want the information to come from someone that I trust because I don't trust unknown medical professionals like the McMoyler Method taught me to do for the first birth. Her method didn't work out so well for me. I want a doula to help protect my environment while I focus on my baby.
Zack and I interviewed six doulas and they were all wonderful and more than qualified for the job. Each interview happened at 8pm in our living room and lasted about an hour. We didn't have a list of questions. We just chatted with each doula and got to know them. Zack and I liked them all. We wrote down all the things that stood out about each one while doing the dishes after they left.
Each doula has something unique to offer and they are all very bright and interesting people. Britt has had amazing success with hypnobirth and is a prenatal childbirth instructor. Esther was a midwife years ago and has a valuable appreciation for postpartum care. Reise is a Birthing from Within childbirth instructor and prenatal yoga instructor. Spring is an apprentice midwife and massage therapist. Jamae has had two home births herself. And, Kara has attended 150 births. The hardest part will be deciding which one of these amazing women is the best fit for us.
Please share your doula recommendations in the comment section.
Kara Engelbrecht
kara@serpentine.com
http://www.karaengelbrecht.com/
Spring Childers
springcmt@yahoo.com
http://www.thebirthdoula.com/
Britt Fohrman
britt@brittfohrman.com
http://www.brittfohrman.com/
Esther Gallagher
esthergallagher@sbcglobal.net
Reise Tanner
reise@treeinthegarden.com
http://www.seedinthegarden.com/
Jamae Tasker
mamaladysf@gmail.com
Other resources:
http://www.sfdoulagroup.com/birthdoulas.html
http://www.naturalresources-sf.com/resources.html#birthdoulas
My other posts on home birth:
On my blog:
http://www.spinachandhoney.com/search/label/Home%20Birth
On SFGate:
Read some of my other posts about birth here, here, here, here and here.
One of my journal entries this month started off, "I've made a breakthrough! I can visualize a calm birth." All my fear had lifted and I had total confidence that my home birth was going to be quick and manageable.
Then this week, I had an appointment at UCSF to establish a relationship with them as my backup hospital and all my mental strength turned upside down. Fear crept in again. I cried at dinner that night when I told Zack about my appointment. It was so emotional for me to have a traditional OB office appointment. I've only had three home birth midwifery appointments but the difference in care is quite stark. At UCSF, I interacted with three people and had four inch sweat circles under my arms before I even saw the midwife with whom I'd made the appointment. That's four people poking and prodding; and asking sensitive questions.
A midwife-in-training asked me the reason for my last cesarean. I said, "failure to progress, that is why I am doing a home birth." She asked if I or the baby showed any other signs of distress. I said, "No, it was 11:30pm, I had been pushing for three hours, and the doctor had to be called in from Marin so they didn't want it to get too late." She smiled and said, "well, that's CPMC, pushing for three hours is normal for a first baby."
Even though my appointment was just a meet-and-greet, I was shuffled through the routine visit protocol. I peed in a cup and undressed completely. As I sat in a pile of paper on the exam table trying to hold up the paper that had ripped and was falling off my shoulder, I thought, "No regrets." When the midwife came into the room, she said, "Oh, it looks like we asked you to get undressed unnecessarily. We aren't going to do an exam so why don't you get dressed and we'll just sit down and talk for a bit." The rest of the visit went well until the end.
She explained how UCSF works with home birth patients. UCSF views themselves not as a backup but as a parallel caregiver. I can use their advice line, make an appointment at anytime, go on a hospital tour, participate in their pregnancy classes, check-out books from their library; in the event that I do need to go to the hospital, I don't go into the emergency room, I go straight up to the maternity care center. On the record, the doctors don't support home births, but they do support everyone's right and ability to make decisions for themselves. I felt very welcomed and happy to have this new support group. Then, I ask her what her opinion was on vaginal birth at home after a cesarean.
I had planned to ask this question because I don't want to hide from the other side of the coin. I want to listen to all the information out there because that is what has given me the knowledge and security that I need to make the home birth decision. I was prepared for the, "I don't think it's a good idea" response. Or, at least, I thought that I was.
She was very matter of fact about her response and managed to be quite frank without being at all hostile towards me. Her explanation was about ten minutes long. To summarize, she felt that home births were a good choice for women with no advanced warning of a problem. Having had a previous cesarean is an advanced warning, so she does not feel that it is a good choice. She feels like the choice for a home birth with my scar is emotional. And then, there was a long awkward silence.
I did not reply. I agreed with her for the most part. I know that women in my situation with one previous low transverse scar have a 0.6% chance of a uterine rupture, but the risk of a uterine rupture is the same at a hospital and it isn't any greater then a lot of other complications that could happen to anyone. The difference is that I am closer to an operating room if I am already at the hospital. So really everything boils down to the 10 minute drive to the hospital.
Until 1999 the American College of Obstetricians and Gynecologists allowed a maximum response time of 30 minutes for a VBAC emergency cesarean. The guidelines have changed since then but are controversial. It remains 30 minutes in Canada. The American Academy of Family Physicians believes that an emergency management plan is suffice.
And then, there is everything else that needs to be looked at when deciding on a home birth after cesarean. And I believe everything else includes the emotional side too. Birth is not just science and statistics. A woman's emotion and sense of security has a lot to do with it. I believe that I stopped my labor when I saw the nurses roll in three carts of equipment after one of them said the baby was coming.
From what I've read, most uterine ruptures are not explosive and unforeseen. Most of them come with a lot of advanced warnings like pain much different from labor pain, vaginal bleeding, sharp pain between contractions, contractions that slow down or become less intense, abdominal pain or tenderness, recession of the fetal head (baby's head moving back up into the birth canal), bulging under the public bone (baby's head has protruded outside of the uterine scar), and sharp onset of pain at the site of the previous scar. I will be closely monitored and taken to the hospital at the first sign of something out of the normal spectrum.
Uterine ruptures are more likely to happen if I am given pitocin, which I could only get at the hospital. And then, there's the risk of another unnecessary cesarean at the hospital which I am guessing is around 16% (my own estimate current rate, 31.1% - optimal rate, 15%). A second cesarean holds risks to me and my baby that are equally as dangerous as a rupture.
The bottom line for me is I only want to go to hospital if I have to. I need to feel safe to have a successful birth. I trust my body to do what it needs to do and I trust my midwife to take me to hospital if she sees any sign of complications.
So, maybe my encounter with UCSF was a blessing in disguise, it made me doubt my decision for a few hours and force me to study everything again and come to the same conclusion again. Home birth.
Reference for list of uterine rupture signals here.
Read some of my other posts about birth here, here, here, and here.
I had my first trimester combined screening test. Just a couple of years ago it was only offered to woman over 35, but now it is offered to all low-risk women no matter what age. I can read between the lines on this one. Larger pool of people equals more money. Even with this knowledge, I couldn't resist getting the test done. At first I said that I didn't want to do it. I didn't want to get a false positive and have to take other riskier tests to get a clear answer. Plus, I didn't feel like I could abort my baby no matter its condition this late in the pregnancy.
But once these tests are offered to me, I start to worry and the only way to stop the worrying is to take the test. If they were never offered to me, I wouldn't worry because I am healthy and don't have any reason to worry (reasons to worry listed on UCSFs website).
So, I got up at 6:30am to go to my 7:45am combined screening test at UCSF.
Both my home birth midwife and my former OB offered me the test. With both, I needed to take it at a lab outside the my regular care office. I chose UCSF because that is my backup hospital in case my home birth doesn't happen. So far, I've noticed no difference between prenatal midwifery care and OB prenatal care in regards to the medical tests offered to me.
So, I got on my bike and road down the driveway. Oops, flat tire. Back to the garage to drive the car. I was the first to arrive in the waiting room. In fact, I was waiting by the locked office door when the receptionist arrived to open it for the day. As people trickled in they were all with their husbands. My sweet husband was home listening to his weekly staff meeting on speaker phone while playing with our two-year old.
My name was called and I was escorted to a room with a chair that looked like a dentist chair. The room was dark and warm from the humming of the ultrasound machine. On the wall was a TV monitor. Soon my baby was on it like a reality TV show that it didn't sign up for. I smiled, happy to see it swimming around. But after five minutes, I closed my eyes and sleep washed over me.
The test consisted of taking pictures and measurements of the baby. The technician tried to keep my attention by pointing out the hands and the feet but soon stopped when she realized that I wasn't opening my eyes.
After the ultrasound, she pricked my finger to draw a few drops of blood to be sent to the lab. As I was leaving, she suggested that I bring my husband next time. Maybe she thought that at least someone sould enjoy the expensive showing of my fetus.
When I got the phone call with my results a week later, the lady said my risks were as if I was 20-years old. I can't remember the stats but they were like 1 in 500,000. So, I am really low risk for having a down syndrome baby.
My worrying has stopped so that seems to make it all worth it. I have had a pleasant few weeks without appointments and have just been enjoying being pregnant. Although I started to worry that I feel small for 20 weeks. I'll have to ask Maria about that at my second home birth prenatal appointment tomorrow.
Read some of my other posts about birth here, here and here.
Maria didn't quote any study. She only said that she wouldn't be doing midwifery if she thought it was unsafe. "I really don't sugar coat any of it, because in reality, we could be dealing with some very hard scenarios at home that require guts and grit and trust in one another." I got the feeling that Maria expects her clients to be well informed when they walk in her door. In her office, she was not promoting the home birth cause or trying to convince me of a home birth. However, I do know from reading her blog that outside her office, she does do an enormous amount to help get the word out that home birth is a safe option for childbirth. Nonetheless, if I hadn't spent the last two years of my life researching birth, I think that those forms might have scared me away.
When I took my husband, Zack, to the informational interview, I had done a ton of research but Zack hadn't done any. I was hoping that she would give him a crash course in all things home birth. Instead, she only went over the risks. I left feeling like I would certainly never have a home birth now, but Zack didn't feel the same way and so here we are.
For me, the turning point was Maria's non-cavalier approach. If my birth is continuing normal, normal, normal, I can stay at home. The minute the baby's heart rate changes or my labor stalls or the birth has moved out of the normal spectrum, she takes me to the hospital. This approach makes sense to me, take me to the hospital only if there is something that doesn't seem quite right.
Then she presents the money forms. All prenatal, birth, and postpartum care is $4,000. If an ultra sound at 20 weeks shows that I have placenta previa, then the safest thing to do is to have my baby at a hospital and she will just charge me for my appointments up to that point. So, my whole birth plan could change in a couple weeks when I do my 20-week ultrasound. My insurance will cover 70% of the $4,000. Our expenses will be less than my total co-payments from my last birth.
She also provides a model of care that would transfer a woman to the hospital at 8 centimeters. So, I could do all the luxuriousness, hour-long prenatal appointments, labor at home with her monitoring me, and then go to the hospital. Then receive the postpartum appointments after the birth. So, it's like home birth care but with a hospital transfer at 8 centimeters. I thought this could be a lovely option for some, but if I make it to 8 centimeters at home and everything is looking good, no way do I want to get in a car and go to the hospital.
Next came the fun stuff and Maria took off her game face and I had the most enjoyable prenatal appointment. We listened to the baby's heart beat and marveled at its strength. She didn't tell me that I was still in the first trimester and a miscarriage was still possible even with an active baby and strong heart beat, which my last visit with an obstetrician told me. Midwifery care allows me to enjoy being pregnant. Let me worry only when there is something to worry about. Then, I had my blood drawn; I peed in a cup. All the usual stuff. Every few minutes a two-year old from the adjoining chiropractic office would peep his head under the curtain. Beautiful works of art about birth and pregnancy filled the walls. In a corner of the room, there is a place set-up for children to play with wood toys.
Read some of my other posts about my first child's birth here and here.
I was "complete." The nurse said, "the baby is coming." And then something spooked me and my cervix closed up to 6 centimeters. I think that it might have been the gear that they rolled in at that moment. There was so much stuff for a little baby not in distress that it could have filled the back of a pick-up truck. In Ina May's, Guide to Childbirth book she talks a lot about how women are so sensitive during childbirth that something as small as an unhappy thought can stop her labor.
When I heard six centimeters after being told that the baby was coming, I thought that I'd have to redo the hours of labor that it took me to get from 6 to 10 centimeters. In fact, according to Ina May, a woman can quickly dialated back to 10 centimeters in very little time if the cause of her distress is eliminated. I confirmed this with Hokhmah K. Gandley, a San Francisco family nurse practitioner and nurse midwife.
If I had known that I could quickly dialate back to 10 centimeters, I think that I would have had the courage to continue without an epidural. Instead, I got the epidural and the whole domino affect of interventions that follows. I ended up with a non-emergency Cesarean section at around midnight. In a postpartum appointment, I asked if there was anything else that could have been done to avoid the surgery. My health care professional said that I could have pushed longer but it was midnight and everyone wanted to go home.
Read my other post about birth here.
For the past year and a half since Mikey was born, I have pondered food. Today as I contemplate having a second child, I am seeing a similarity between the food industry and the birthing industry. Strange, I realized, but read on.
Mikey was born in a hospital by cesarean section. While in labor but before my surgery, I was given everything on the modern medicine's menu. I remember saying, "Look sweety, do you see that, the lights are rabbits."Before I started taking food seriously, I thought it was normal to feed children Gold Fish and Cheerios, but now I don't think that these foods are really food at all.
Like food, I am starting to question how normal it really is to give birth in a hospital. Having a baby isn't an illness. I am starting to question the whole concept of going to the hospital just like I started to question what I was feeding my baby.Our nation started having babies in the hospital around the same time we started eating processed food (early in the 20th century). How did my great grandmother give birth to my grandmother and all those women before her? And, are women better off in the hospitals today then they were before hospitals? Is there less infant mortality now or then? From what I've read, we are certainly not healthier eating chips, soda and other processed foods. Are we better off giving birth in a hospital or not?
Giving birth without a doctor or hospital wasn't even a consideration for me back when Mikey was born, but now that I have had the hospital experience, I am not sure that I want to repeat it. There are plenty of recent reputable studies out there saying we shouldn't be eating most of what is being sold to us in the grocery store, but it is still there ready to take our money. Are we just going to hospitals to give birth because that's just what we do or is it actually the right choice?Although it seems like it's a far fetched comparison, could giving birth in the hospital be equally unhealthy as buying processed foods at the store? Are hospitals, like food companies, taking the control from the mother and putting it in the hands of the so-called experts?
When I didn't know better, I thought, "Why would all this food be sold if it were harmful to my health?" Well, from the books that I’ve read, it's quite clear that no one is looking out for me. We are sicker as a nation then ever before and it is in short because of these replacement foods.Today, I think about hospitals the same way that I use to think about the aisles and aisles of industrialized food. Hospitals know best. They are first and foremost looking out for me and my interests. However, since the traumatizing birth of my son, I have started to doubt this unscrutinizing faith in hospitals. Why did the birth of my son take me five months to physically recover and two years to mentally recover?
Are hospitals becoming too big of a business to do what's in the best interest of us moms?Mikey was born by cesarean. The whole experience was so traumatic that I can't talk about it without crying. I believe that everyone in my delivery room was doing the best that they knew how to keep me and Mikey safe and grant me a natural birth, but even knowing this, I am still upset. The sad thing is that the women who have witnessed my embarrassing breakdown, say that they feel the same way about their birth experience.
In the film, Ricki Lake offers another point of view. By using some shocking images, she captures the viewers attention. And then, she urges us to realize that our bodies know how to have babies and shows us that having a baby is not a medical condition that needs treatment. Her film gave me courage and the extra push to try for another natural birth.
Maybe it was my cesarean surgery that made me realize that I need to listen to myself and believe in what I know is right instinctually for me and my son. It gave me the strength to go against the grain with nutrition. It sounds a bit like Al Gore's message on climate change. The human race cannot continue on the path that it is on. We can't continue eating poor food, we can't continue having children by drugs and/or major abdominal surgery, we can't continue stressing our fragile ecosystems. Each individual person has the power to make change at least for themselves and their children. Let's take responsibility for our health, our children and our earth. It is not someone else's job, it is our job.
The Business of Being Born
http://www.thebusinessofbeingborn.com/about.htm
International Cesarean Awareness Network
http://ican-online.net/index.php?option=com_frontpage&Itemid=1


